Digital Health Care Market Study — Part 1
June 23, 2022
-
Copyright and permission to reproduce
This publication is not a legal document. It is intended to provide general information and is provided for convenience. To learn more, please refer to the full text of the Acts or contact the Competition Bureau.
For information on the Competition Bureau's activities, please contact:
Information Centre
Competition Bureau
50 Victoria Street
Gatineau QC K1A 0C9Telephone: 819‑997‑4282
Telephone (toll-free in Canada): 1-800-348-5358
TTY (for hearing impaired): 1‑866‑694‑8389
Fax: 819‑997‑0324
Website: www.competitionbureau.gc.caThis publication can be made available in alternative formats upon request. Contact the Competition Bureau's Information Centre at the numbers listed above.
Permission to reproduce
Except as otherwise specifically noted, the information in this publication may be reproduced, in part or in whole and by any means, without charge or further permission from the Competition Bureau, provided that due diligence is exercised in ensuring the accuracy of the information reproduced; that the Competition Bureau is identified as the source institution; and that the reproduction is not represented as an official version of the information reproduced or as having been made in affiliation with, or with the endorsement of, the Competition Bureau.
For permission to reproduce the information in this publication for commercial purposes, please fill out the Application for Crown Copyright Clearance or contact the ISED Citizen Services Centre mentioned below.
ISED Citizen Services Centre
Innovation, Science and Economic Development Canada
C.D. Howe Building
235 Queen Street
Ottawa, ON K1A 0H5
CanadaTelephone (toll-free in Canada): 1‑800‑328‑6189
Telephone (international): 613‑954‑5031
TTY (for hearing impaired): 1‑866‑694‑8389
Business hours: 8:30 a.m. to 5:00 p.m. (Eastern Time)
Email: ISED@ised-isde.gc.ca© Her Majesty the Queen in Right of Canada, as represented by the Minister of Industry, 2022.
Date: 2022-06-20
Aussi offert en français sous le titre Libérer la puissance des données de santé — Étude de marché sur les services de santé numériques — Première partie.
Foreword
Remember when your doctor’s office was burdened with seemingly endless shelves of paper medical files? For the most part, that’s no longer the case. Most patient information is now stored electronically in digital systems, which have become an essential part of health care information management. But there are limitations to these systems. They often can’t exchange information with other systems, making it difficult for patients and health care providers to access and share personal health information.
What does this have to do with competition in Canada?
When it’s difficult to securely access and share personal health information, it’s harder for patients and health care providers to use new, efficient digital health care solutions. This could include things like e-pharmacy platforms, virtual care, mobile health care apps and wearable devices. This, in turn, makes it harder for the digital health care innovators and start-ups to enter the market with viable solutions. That hurts competition and innovation in Canada.
More needs to be done to help unlock the power of personal health information – so that Canada’s digital health care sector can fully benefit from competition.
There are practical ways to increase competition in this area. For instance, governments can allow secure access and sharing of patient information, while putting rules in place to protect privacy and ensure patient consent. Doing so invites a more competitive environment for companies to enter the market with new, cutting-edge digital solutions to better serve Canadian patients and health care providers.
Table of Contents
Executive summary
This report makes major recommendations to Canadian policymakers on ways to make it easier to access and share personal health information—securely and efficiently—to benefit competition. More competition helps ensure Canadian patients and health care providers have access to new, innovative digital health care solutions.
Canadians and their health care providers should be able to access and share their personal health information and do so easily and securely. But that’s not the case currently.
Most Canadians’ personal health information is stored in databases called electronic medical records (EMRs). There are many types of EMRs used in various settings, such as hospitals or by specialists. This report focuses on primary health care EMRs, used by family doctors and other primary health care providers to store information, such as medical histories and lab results.
In Canada, the majority of health care providers use a primary health care EMR system owned by one of three companies. Accessing and sharing information from those systems is often difficult. As a result, much of Canadians’ personal health information is locked inside the systems of a small number of companies.
There are a number of barriers that make it hard for new companies that make EMR systems and other digital health care solutions, like virtual care and e-pharmacy solutions, to enter the Canadian market. We study two major barriers in this report:
- Disparate privacy and data governance rules across provinces and territories. This can prevent new digital health care solutions from succeeding: making it harder and more expensive for them to enter multiple provinces and territories. This makes Canada less attractive to digital health care entrants that could bring more competitive vigor and innovative solutions to the market. It also makes it difficult to share personal health information across jurisdictions.
- Difficultly accessing personal health information contained in primary health care EMR systems. This makes it harder for health care providers and patients to adopt new and innovative digital health solutions: making it difficult for them to access and share information. For the companies that develop those solutions, it limits their ability to gain a foothold in the market and compete with existing players. This can hurt long-term innovation and deter start-ups.
These barriers can reduce data sharing among health care providers, impede innovation and lower the adoption of digital health care solutions. Primary health care EMR systems should instead be interoperable. Interoperability enables information to flow seamlessly between different solutions. That can allow personal health information to be seamlessly shared between health care providers and digital health care solutions, with appropriate privacy and security protections in place. This can spur greater competition for digital health care solutions and unlock the power of personal health information.
- Harmonize privacy and data governance rules across Canada.
- Require primary health care EMR companies to comply with “anti-blocking” rules.
- Require access on a fair, reasonable and non-discriminatory (FRAND) basis.
- Put an independent organization in place to establish and enforce anti-blocking rules.
- Create incentives to encourage compliance with anti-blocking rules.
- Require that data be shared effectively in a useable format for other companies.
- Require that the cost of data sharing be reasonable.
- Establish interoperability standards for primary health care EMR systems.
- Put an independent organization in place to establish, implement and enforce interoperability standards.
- Create incentives to encourage compliance with interoperability standards.
- Implement interoperability standards that are not rigid.
- Use regulatory sandboxes to assess potential risks to data quality, security and privacy.
- Eventually extend primary health care EMR interoperability standards to EMRs used in other health care settings.
About the Competition Bureau
The Competition Bureau (“the Bureau”) is an independent law enforcement agency that protects and promotes competition for the benefit of Canadian consumers and businesses. Competition drives lower prices and innovation while fueling economic growth.
As part of its mandate, the Bureau advocates to policymakers for increased competition in regulated sectors of the economy, such as health care, telecommunications and banking. This report forms part of a market study that the Bureau has undertaken to support this goal. Market studies allow the Bureau to apply a competition lens to a range of industries it examines. This type of analysis helps highlight issues that may restrict competition and recommend solutions to policymakers for the benefit Canadians.
In this report, the Bureau reviews competition in a specific part of the Canadian health care sector and provides recommendations to policymakers to encourage greater choice and innovation.Footnote 1
Methodology
To inform its study, the Bureau gathered information from a range of primary and secondary sources. The study draws from public research, journalism and other reports. It also incorporates confidential informationFootnote 2 shared with the Bureau by companies, governments and consumers.
The Bureau conducted more than 50 interviews, received 42 written submissions and heard from 425 Canadians through an online survey.
The Bureau thanks everyone who took time to provide information and to help advance this important study.
The challenge facing Canada
Key takeaways
- Personal health information is critical to patient care. It helps patients make better decisions about their health and allows health care providers to improve patient care. Much of this information is stored in primary health care EMR systems.
- It’s hard for patients, health care providers and industry to securely access personal health information stored in primary health care EMR systems. It limits how much Canada’s health care system can unlock the full value of personal health information.
- Interoperability can allow personal health information to be shared across different digital health care solutions, with appropriate privacy and security protections in place. This means better, more innovative digital health care solutions for health care providers and Canadians.
Innovation lags in health care today
While digital technologies have reshaped Canada’s economy, such innovation in Canadian health care currently lags behind other sectors. When it comes to health care, many Canadians still must fill out paper forms at clinics and wait on faxed prescriptions at pharmacies.
The COVID pandemic quickly brought the value of digital health care services into sharper focus. What were once niche solutions, such as virtual care (visits with a health care provider by phone or video) and e-prescribing, became essential to Canadians. Today, health care providers, patients and health care companies are embracing the convenience and value of these new digital products and services.Footnote 3 Nevertheless, Canada is still playing catch-up compared to many other countries.
The challenge facing digital health care in Canada is not a matter of lacking a supply of reliable data or technologies. Studies suggest health care produces nearly 30% of the world's data.Footnote 4 Yet health care systems here are data rich but information poor: there’s plenty of data being created, but it’s not being used effectively.Footnote 5
In Canada, personal health information is used differently across provinces and territories. Even within those jurisdictions, health care organizations (e.g., health authorities, hospital systems, community health centers) don’t all treat personal health information the same way.
Health care systems here tend to be siloed, making it difficult to share data. Privacy frameworks are generally built on a provincial or territorial level and often differ from one place to another. Rules governing the use of data, for example the use of anonymized data for clinical research, also vary between jurisdictions. As a result, health data systems in Canada often can’t “speak to each other.” This hurts innovation in the health care sector.Footnote 6
Studies show Canada lags behind its peers in solving this problem. A 2019 Commonwealth Fund survey of physicians ranked Canada near last in terms of using digital health care solutions.Footnote 7 Canada trailed New Zealand, Sweden, the U.K., and the U.S. in providing virtual care. This includes video consultations and viewing test results online. Canada also performed poorly in allowing health care providers to digitally share personal health information.
Canadians want digital access to their personal health information, but such access is often not available and incomplete. A 2021 survey by Canada Health Infoway found that eight in ten Canadians wanted to access their personal health information online. However, that same survey shows only three in ten could do this.Footnote 8 COVID accelerated some digital health care solutions, but it also showed that much more needs to be done.

The ability to combine data from disparate sources and draw new insights opens the door to competition from new solutions, such as precision medicine (i.e., leveraging the power of artificial intelligence, big data, genomics and population health). Progress in this area will result in more personalized treatment and better ways to care for all patients.Footnote 9
Electronic medical records

-
Figure 2 — Image explaining the use of primary health care electronic medical records (PHC EMRs).
86% of family doctors use PHC EMRs, and 25% exchange patient summaries electronically with other doctors.
Information stored in PHC EMRs:
- Demographics
- Diagnoses
- Family history
- Allergies
- Immunization
- Medications
- Procedures
- Lab results
Electronic medical records (EMRs) contain personal health information gathered by a patient’s health care provider. They are the digital versions of the paper charts commonly used in clinics and hospitals.Footnote 10 There are many types of EMRs used in different health care settings, such as hospitals or by specialists. Primary health care EMRs contain personal health information collected in a family doctor’s office or other primary health care setting. It includes patient histories, allergies, visit notes and medication history. Nearly all Canadian family doctors store patient data in primary health care EMR systems. But it’s rarely shared with other providers. Only a quarter of doctors share patient summaries digitally. Only about one third share lab results or medication lists. Only 5% allow patients to view their information online. share lab results or medication lists. Only 5% allow patients to view their information online.Footnote 11
Canada’s primary health care EMR market is highly concentrated, with only two or three companies accounting for nearly all the market share in most provinces and territories. This means much of Canadians’ personal health information is held by a small number of large companies.
Currently, the leading primary health care EMR companies are: TELUS Health, QHR Technologies (owned by Loblaw Companies) and WELL Health Technologies. Collectively, they have as much as a 100% share of the market in some provinces.Footnote 12

-
Figure 3 — Share of community clinics by certified EMR vendor in Ontario and Saskatchewan
Ontario
- TELUS: 42%
- QHR: 26%
- WELL: 39%
- Other: 30%
Saskatchewan
- QHR: 80%
- TELUS: 20%
Primary health care EMR companies continue to grow through acquisition. Some of these acquisitions involve competing primary health care EMR companies. Others involve related products used to provide services such as virtual doctor visits and e-pharmacies. Others have involved purchases of brick-and-mortar physician practices, health clinics, and pharmacies.
For example:
- TELUS acquired EMR providers Med Access, Medesync and Nightingale. TELUS also acquired virtual health care solutions, including Babylon, Akira Health and EQ Care. They also purchased pharmacy management software, including XD3 Solutions.
- QHR acquired EMR providers Accuro and Jonoke. They also acquired virtual health care solutions, including Medeo.
- WELL acquired EMR providers Trinity Healthcare, OpenHealth and ClearMedica. They also acquired virtual health care solutions, including INSIG. WELL is also the largest integrator of open-source OSCAR EMR solutions.
Interoperability
Interoperability allows personal health information to be shared across different digital solutions. When systems interoperate effectively, health care providers from different clinics can access, add and exchange patient data with one another. It allows for greater cooperation between health care providers, while ensuring that current information is available.
There are two forms of interoperability:
- Horizontal interoperability, which means competing systems can communicate with one another. For example, information in one primary health care EMR system can be viewed, updated and edited in another.
- Vertical interoperability, which means one system can provide information to a related system. For example, appropriate information in a primary health care EMR system can be viewed, updated and edited in pharmacy software to ensure that a pharmacist has access to accurate and up-to-date information about a patient’s medications.Footnote 13

-
Figure 4 — Horizontal and vertical interoperability
Three images comparing how information can be transferred by one-time transfer, by horizontal interoperability and by vertical interoperability. The first image shows that a one-time transfer involves one EMR sending information to another EMR. The second image shows that horizontal interoperability allows two EMRs to transfer information back and forth between them. The third image shows that vertical interoperability allows the transfer of information between an EMR and other digital health care solutions.
For two systems to be interoperable, they require a common language. This can be done by using a web service or an application programming interface (API). When digital health solutions offer API access to third parties, it allows those third parties to obtain personal health information from the platform in use.Footnote 14
When primary health care EMR systems are made interoperable, it’s easier for the digital health care innovators and start-ups to enter the market and compete with existing companies. It also results in important benefits for patients, health care providers and the health care system.Footnote 15 These benefits include:
- Empowering patients to:
- Take greater control of their health by giving them access to the information they need to make informed choices.
- Add or correct information in their record.
- Make it easier to provide care for family members.
- Make it easier to communicate with their circle of health care providers.
- Empowering health care providers to:
- Access consistent and timely personal health information to tailor and coordinate care.
- Make use of aggregated personal health information to improve quality of care and patient safety, and easily identify at-risk and complex population groups to better target their care.
- Save time, lower costs and improve operational efficiency by taking advantage of modern digital tools.
- Reducing duplication, for example of tests and procedures, and wasted effort within the health care system, thus saving time and money.
- Improving public health policies. This includes being better at targeting disease prevention and responses to public health issues.
Many countries have created national standards to promote sharing of personal health information. For example:
- In the U.S., the 21st Century Cures Act (Final Rule) requires health care providers and companies to enable patients’ access to their personal health information securely and easily. Patients have the option to do this through an app they authorize.Footnote 16
- In Australia, the federal government created “My Health Record,” a national electronic record for all citizens. It collects summaries of personal health information for various health care providers to access. Patients and their approved representatives can also access personal health information, including by using approved third-party apps. It also supports the use of this information (with patient consent) for research and public health.Footnote 17
- In the U.K., the National Health Service’s “Spine” compiles personal health information from different providers in a single database. The Spine information is accessible to both providers and patients, including through an online app or portal. To support app developers working on this project, test environments and data are available.Footnote 18
The U.S. Office of the National Coordinator for Health IT (ONC) outlines three criteria for health systems to be considered interoperable.Footnote 19 The software must:
- Securely exchange electronic health information with another technology. It must then be able to use this information without special effort on the part of the user.
- Allow complete access, exchange and use of all electronic health information.
- Not engage in information blocking. This means it must not prevent or substantially discourage the access, exchange or use of electronic health information.
No similar systems exist in Canada. Most provinces and territories do not have provincial patient portals, so any data available is provided by individual health care organisations, providers or companies, and is therefore siloed. Some provinces and territories have developed portals that allow patients to access their personal health information. However, the data in these systems are often incomplete and do not cross provincial or territorial borders. Therefore, they offer only limited personal health information sharing.Footnote 20
There have been efforts in Canada to make primary health care EMR systems work together. Yet these efforts have not resulted in a workable set of national standards. Where current systems are interoperable, it’s done only in a limited way.
Current progress toward interoperability in Canada can be summarized as follows:
- Primary health care EMR companies have no financial incentive nor are they required by law to be interoperable. As a result, personal health information is often not shared. Instead, it remains siloed in primary health care EMR systems.
- In some health care settings, EMR companies are required to provide interoperability. But most of these efforts have not yet focused on primary health care EMR systems. Moreover, provinces may sometimes modify these rules to meet local requirements. This can stop data from being shared with other regions. A patchwork of rules from one region to the next can also increase company compliance costs and cause confusion.
- Canada Health Infoway (CHI) is a federally funded non-profit that works to aid interoperability. CHI aids the industry in the form of financial support, working groups and technical advice. CHI could play a more central role to develop national standards that make primary health care EMR systems more interoperable. They could also work to incentivize companies’ alignment with standards.
- Standards alone are not enough to ensure workable interoperability between primary health care EMR systems. Companies may meet required standards, but still prevent meaningful personal health information exchange. This is why explicit anti-blocking rules are also required.
- Health care providers are the custodians of personal health information. Yet they are not incentivized to invest in data management or share the information they collect. As a result, personal health information held within primary health care EMR systems is often of poor quality and may be kept in non-standard formats that hampers interoperability. Governments often work to enable health care providers to receive personal health information into their EMRs. However, this work is not necessarily focused on sharing that data with others.
- Third-party digital health care solutions are often unable to access a patient’s personal health information. Instead, patients are required to collect and compile this information themselves from many sources. Some of these sources are often paper based, requiring that information be subsequently digitized.
Provinces and territories have taken unique paths to make primary health care EMR systems interoperate. Highlights of their strategies and outcomes include:
- Primary health care EMR certification. Several provinces require primary health care EMR systems to be certified. This means a system must be approved before it can integrate with provincial and territorial electronic health record systems, which combine information from multiple EMRs. Examples include: Ontario, Quebec and Manitoba. Health care providers rarely opt for uncertified EMRs.
- Single primary health care EMR market. Some provinces identify a single primary health care EMR company for all health care providers. This may address the challenge of ensuring that health care providers’ systems are interoperable. Examples include: Newfoundland and Labrador, Prince Edward Island, the Northwest Territories and Nunavut. New Brunswick previously had a single primary health care EMR market, but recently moved to adopt an EMR certification process.
- Decentralized or unregulated primary health care EMR market. After having discontinued its single primary health care EMR program, British Columbia now has nine primary health care EMR companies in use that are not regulated in terms of interoperability standards.
- Regulatory and legislative reform. Some provinces use legal tools to ensure personal health information systems interoperate. Examples include:
- Ontario recently created its Digital Health Information Exchange Standard (DHIEX). This regulation requires health care providers to use interoperable systems.
- Quebec adopted legislation Bill 64, “An Act to modernize legislative provisions as regards the protection of personal information.” It updates Quebec’s personal data protection framework and is intended to improve patient access to personal health information. It is also meant to enable personal health information use for research and innovation.
Making the Case for Competition
Key takeaways
- In Canada, personal health information is too often locked inside a proprietary system of a specific primary health care EMR company. It stops personal health information from being shared, which in turn: undermines its value potential; impedes innovation; and lowers the adoption rate of digital health care solutions.
- The current regulatory landscape in Canada makes it hard for companies that make EMRs and other digital health care solutions (e.g., virtual care and e-pharmacy solutions) to enter the Canadian market. Major barriers include:
- Disparate privacy and data governance rules across provinces and territories.
- Difficultly accessing personal health information contained in primary health care EMR systems.
- Three recommendations are made in support of greater competition in this important area of the Canadian economy.
Why competition matters
Competition is the driving force of Canada’s economy. It pushes companies to build better products and find new ways to earn customers. Competitive markets are needed now more than ever to deliver low prices, more choice and increased innovation for Canadians. Competition in health care—as with other sectors—makes the economy more productive and innovative…so everyone wins.
More competition between primary health care EMR companies has similar effects. It can lead to better choices for health care providers and more opportunities for new, innovative solutions. One way to enhance competition among primary health care EMRs is by making it easier to access and share the personal health information stored within them—securely and efficiently. This can attract more companies to enter the market, expand and invest in research and development.
Barriers to competition
There are two major barriers to address in the area of personal health information:
Disparate privacy and data governance rules across provinces and territories.
Primary health care EMR companies face several challenges when competing in Canada. The most common one: having to contend with a differing set of rules across provinces and territories. This absence of a single set of rules creates structural inefficiencies and barriers to growth for primary health care EMR companies. They instead must deal with a patchwork of privacy laws, certification rules and technical requirements—all of which must be satisfied. The net result is a complex environment that makes it difficult for companies to enter and expand in Canada.
High entry costs. Each province and territory has its own set of privacy and data governance rules that companies must meet. This requires EMR systems to be customized at the provincial/territorial level. Customization is costly, and these additional costs make entry less likely. This is especially true in smaller jurisdictions, where there is less of a user base across which to spread costs. A patchwork of rules from one region to the next makes it harder for domestic companies trying to scale-up to compete at a national or even international level. It can also deter foreign companies from entering Canada because of the inability to enter at a national level. This is because they have to incur an additional set of costs for each jurisdiction entered.
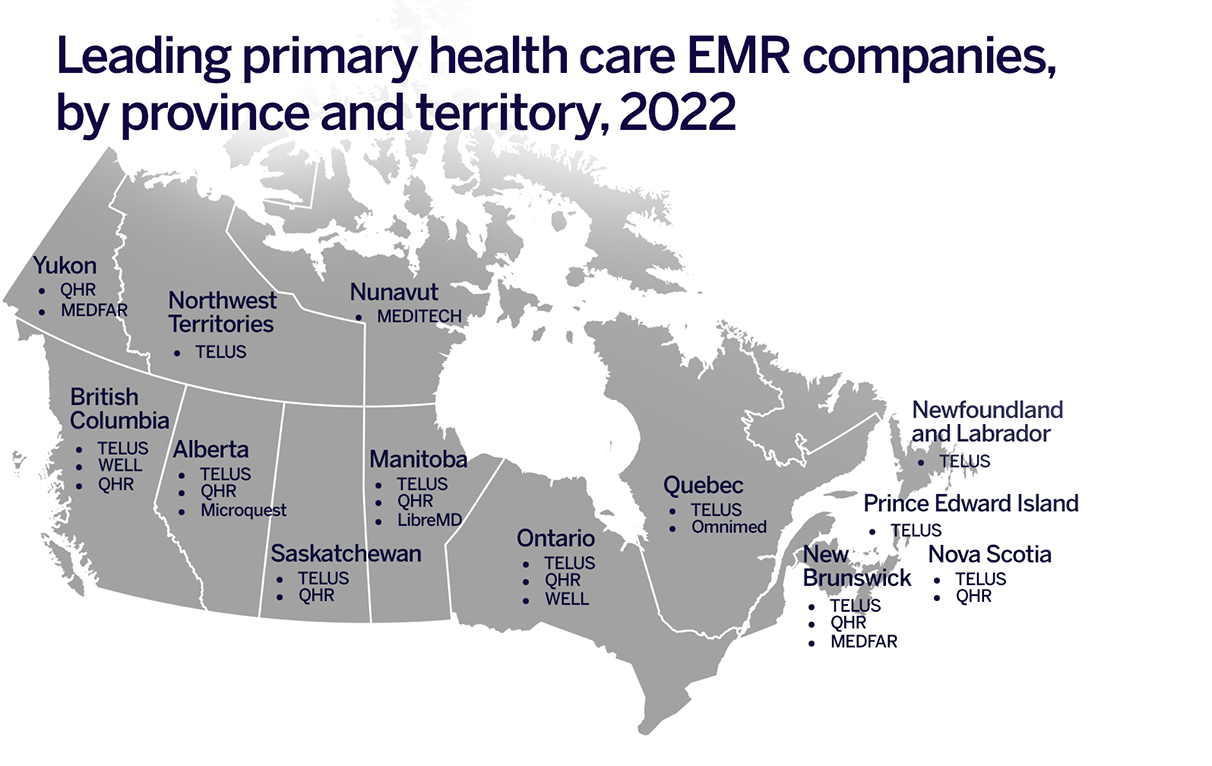
Market fragmentation. A key strength of digital products is that they can be distributed easily across borders. However, that benefit is not fully realized for personal health information in Canada, due to the lack of common rules for primary health care EMR companies. The result: fewer companies that compete in every part of the country. This can be seen in the number of region-specific primary health care EMR companies in Canada (see illustration below).
-
Figure 5 — Leading primary health care EMR companies, by province and territory, 2022
A map of Canada listing the leading primary health care EMR companies in each province and territory.
Territories from west to east:
Yukon
- QHR
- MEDFAR
Northwest Territories
- TELUS
Nunavut
- MEDITECH
Provinces from west to east:
British Columbia
- TELUS
- WELL
- QHR
Alberta
- TELUS
- QHR
- Microquest
Saskatchewan
- TELUS
- QHR
Manitoba
- TELUS
- QHR
- LibreMD
Ontario
- TELUS
- QHR
- WELL
Quebec
- TELUS
- Omnimed
- MEDFAR
New Brunswick
- TELUS
- QHR
- MEDFAR
Prince Edward Island
- TELUS
Nova Scotia
- TELUS
- QHR
Newfoundland and Labrador
- TELUS
Difficulty accessing information contained in primary health care EMR systems.
This barrier limits innovation and slows down much-needed adoption of digital health care in Canada. There are three primary situations where challenges occur.
One-time transfers of information from primary health care EMR systems. Being able to directly transfer data makes it easier to switch between companiesFootnote 21. But with many primary health care EMR systems, personal health information is often locked-in, either inadvertently or by design, to the specific system the health care provider has chosen. That makes it difficult for a health care provider to switch to a competing EMR companyFootnote 22. This effect is called a switching cost and it can dampen competition among EMR companies.
Switching EMR systems is a disruptive, time-intensive and expensive process. There are significant financial costs and workflow interruptions associated with having to select, purchase, implement and maintain a new system. These tasks pull health care providers away from treating patients.
These challenges are compounded when health care providers also face uncertainty associated with extracting and transferring personal health information. When health care providers do switch EMRs companies, the old company is often responsible for transferring existing data into the new system. There’s often friction with that process. A number of primary health care EMR companies describe instances where an outgoing company was uncooperative in transferring personal health information. Anecdotes include companies charging high fees, delaying the transfer process or not providing all personal health information in a useable format.
If the switching process is problematic, health care providers may be disinclined to take on the time and expense. This reluctance to switch can ultimately make it less valuable for new EMR companies to enter a market. When fewer health care providers are willing to switch—even when a newer, cheaper or better alternative is available—health care providers end up being locked-in to an inferior system.
Continuous information sharing between primary health care EMR systems. Patients often see multiple health care providers at once. But when their EMR systems don’t interoperate, it’s hard to share information across health care providers—negatively affecting quality of care. The effect is magnified when only a small number of primary health care EMR systems are in use. When a primary health care EMR company gains a large customer base, it can make alternatives seem unattractive. This can prevent competing EMR companies from entering or expanding. These barriers are made even worse where large companies acquire an interest in community clinics, thereby bolstering their user base and making it harder for competing EMR systems to gain a foothold.
Continuous information sharing involving other digital health care solutions. When health care providers adopt new health care technologies such as virtual care and e-pharmacy platforms, those solutions need to be integrated with existing primary health care EMR systems. This makes interoperability even more important.
Many primary health care EMR companies are working to support vertical interoperability across their own proprietary solutions. This could involve sharing personal health information between a primary health care EMR system and a virtual care platform. When an EMR company acquires an interest in a digital health care solution, they further expand their network of affiliated software, systems and apps.
Primary health care EMR companies may pursue a strategy of creating an open ecosystem. Under this approach, other companies are encouraged to readily integrate with the primary health care EMR system, with privacy and security protections in place. This often requires the use of open standards, such as published and external APIs.
Alternately, primary health care EMR companies may opt for a closed ecosystem: a walled garden strategy. This allows the primary health care EMR company to control which third-party solutions are permitted to interface within the ecosystem. While navigating over the wall might still be possible, most EMR users opt to keep things simple and get what they need from within the garden (i.e., existing solution). Thus, a company with a walled garden is able to act as a gatekeeper, controlling: the conditions for third-party access, the type of personal health information being accessed, and the purposes for which it could be used. That gives them much control over the digital health care marketplace and creates a power imbalance between EMR companies and third parties.
Some market participants are concerned primary health care EMR companies are assuming this gatekeeper role. They say this limits their ability to gain a foothold with health care providers. It also constrains their ability to develop, launch and expand new digital health care solutions in Canada.
Recommendation
To unlock the full value of personal health information, primary health care EMR systems should be required to interoperate with other EMRs and digital health care solutions. To do this, governments must ensure all primary health care EMR systems work with a common language. This will enable otherwise-disparate systems to communicate with each other. In doing so, the marketplace can deliver greater competition, innovation and meaningful choices to Canadians.
Therefore, the Bureau has three major recommendations to help foster greater competition in the area of personal health information in Canada.
Recommendation 1
Harmonize privacy and data governance rules across Canada.
Today, there are disparate privacy and data governance rules in each province and territory. The need to customize digital health care solutions to regional requirements further fragments the already small Canadian market. Harmonizing rules across the country will support greater competition. It will simplify entry and market expansion for companies and make it easier for domestic companies to scale-up and compete nationally and internationally. Those changes will help lower prices, boost the range of meaningful choices and drive innovation forward in this sector of the economy.
The OECD made a similar suggestion in 2019Footnote 23. It recommended:
“… governments establish and implement a national health data governance framework to encourage the availability and use of personal health data to serve health-related public interest purposes while promoting the protection of privacy, personal health data and data security.”Footnote 24
The OECD’s report provides guidance on how to develop a national health data plan. This guidance was approved by all OECD countries, including Canada. That report can serve as a useful roadmap for harmonizing rules in Canada. Establishing a viable framework would require provinces and territories to work together toward that united goal.
Recommendation 2
Require primary health care EMR companies to comply with anti-blocking rules.
Anti-blocking rules stop health care companies from interfering with the access, exchange or use of electronic personal health informationFootnote 25. These rules make it easier for health care providers to switch between companies and empowers them to shop around for the primary health care EMR company that best suits their needs. It can also make it easier for Canadians to use new, innovative health care solutions. Together, this can support new solutions entering the market to compete with existing companies. This helps to promote greater innovation in the longer-term.
Other countries are embracing that approach. For instance, the U.S. recently adopted the 21st Century Cures Act. This law creates anti-blocking rules.
Below are highlights of what a similar approach in Canada should entail.
Require access on a fair, reasonable and non-discriminatory (FRAND) basis.
Primary health care EMR companies should be required to make data transferrable to other systems. This is also known as data access on fair, reasonable and non-discriminatory (FRAND) termsFootnote 26.
An independent organization in place to establish and enforce anti-blocking rules.
It’s important that anti-blocking rules be established and enforced by a neutral body. It can comprise members from federal and provincial/territorial jurisdictions. It must be:Footnote 27
- Empowered. It needs resources and the ability to enforce policies.
- Independent and impartial. It must be unbiased. This means it cannot have a commercial interest in—or other ties to—any company for which the policies apply.
- Able to engage and coordinate. It must have the ability to engage with stakeholders and coordinate rules across jurisdictions.
- Able to establish market authority. It must have the expertise to make credible decisions.
Create incentives to encourage compliance with anti-blocking rules.
Governments should put incentives in place to ensure compliance with anti-blocking rules. For example, companies that don’t meet anti-blocking rules could be excluded from certification, government funding or access to provincial and territorial electronic health record systems. Such conditions already exist in some provinces. For example, in Manitoba, when a health care provider switches its EMR solution, the outgoing company is obliged to support the switch. The policy states:
“If a clinician chooses to move to another practice or a practice chooses to change to another EMR product, vendors are required to provide transition services to the affected clinician. These services will access to the clinician’s data by removing all data access restrictions and/or providing him/her with a copy of all his/her EMR data and providing descriptions of the data and the data relationships. Purchasers should be aware that Manitoba does not control the pricing associated with these transition services.”Footnote 28
Ontario and Alberta have similar rules for EMR companiesFootnote 29. Other policies may also be necessary to ensure health care providers have the ability and incentive to share patient health information—with privacy and security protections in place.
Require that data be shared in a format that’s usable by other companies.
There are cases where a one-time data transfer of personal health information is necessary. One example is when a clinic switches from one primary health care EMR company to another. In these cases, the outgoing companies should be required to provide all raw data in an electronic, machine-readable format. This can simplify the process of moving data by limiting burden and reducing costs. It can also ensure no information is excluded in the transfer. However, companies need a common standard to ensure data can be translated from one system to another.
With two-way personal health information sharing between solutions and systems offered by different and even competing companies, primary health care EMR companies should be required to make their systems interoperable (e.g., to make an EMR system work with a competing EMR system or third-party companies). Ensuring this will allow third-party companies to offer better digital health care services to health care providers. But in the absence of rules, there may be little incentive for a primary health care EMR company to do this. To encourage this type of exchange, primary health care EMR companies should be required to enable interoperability, with privacy and security protections in place. Primary health care EMR companies should also provide the same level of interoperability with third-party solutions as they would with their own solutions.
Require that the cost of data sharing be reasonable.
Primary health care EMR companies are likely to incur costs to transfer data and ensure their systems are interoperable. Therefore, it’s reasonable that they be compensated for those costs. The price charged to third-party companies for these services ought to be directly related to those costs. Anti-blocking rules should require that such pricing is transparent and not excessive.
For example, the US Cures Act Final Rule includes a fees exception that “enables actors to charge fees related to the development of technologies and provision of services that enhance interoperability, while not protecting rent-seeking, opportunistic fees, and exclusionary practices that interfere with access, exchange, or use of EHI (electronic health information).”Footnote 30 Key conditions of the exception include that fees charged must:
- Be based on objective and verifiable criteria that are uniformly applied for all similarly situated classes of persons or entities and requests.
- Be reasonably related to the actor’s costs of providing the type of access, exchange, or use of EHI.
- Not be based on whether the requestor or other person is a competitor, potential competitor, or will be using the EHI in a way that facilitates competition with the actor.Footnote 31
Other conditions, such as the timeliness of the primary health care EMR company’s support, should also be considered.
Recommendation 3
Establish interoperability standards for primary health care EMR systems.
The Healthcare Information and Management Systems Society (HIMSS) defines interoperability standards as a “common language and a common set of expectations that enable interoperability between systems and/or devices… regardless of application or market supplier”.Footnote 32 A number of groups and governments have made progress towards defining interoperability standards. However, Canada needs a unified standard to remove barriers to data sharing and promote greater competition.
Horizontal interoperability between primary health care EMR systems can reduce health information silos and improve the ability for health care providers to switch between competing EMR companies. It can support new digital health solutions, improve quality of care and enable health-related research and development.Footnote 33 It can also improve continuity of care, increase efficiency within the health care system and reduce medical errors by ensuring health care providers have access to a complete picture of a patient’s health information.Footnote 34
Vertical interoperability of primary health care EMR systems unties a health care provider’s choice of EMR company from its choice of other related solutions. Health care providers then gain the flexibility to choose the best solution for them without being tied-in to potentially inferior alternatives.
Below are highlights of what such an approach should entail.
Put an independent organization in place to establish, enforce and operationalize interoperability standards.
Like anti-blocking rules, data sharing rules should be established, enforced and operationalized by a neutral body. This body should share the same features as those identified in respect of anti-blocking rules. It can be made up of members from both federal and provincial/territorial jurisdictions. The body must be empowered, commercially independent and impartial, able to engage and coordinate and have all necessary expertise.
Create incentives to encourage compliance with interoperability standards.
As with anti-blocking rules, governments must put incentives in place to ensure compliance with interoperability standards. For example, companies that don’t comply with interoperability standards could be excluded from certification, government funding or access to provincial and territorial electronic health record systems.
There’s already a push to make this happen. Companies that sell in Ontario must meet a common set of rules.Footnote 35 Also, as of 2020, Ontario requires digital health systems to be made interoperable.Footnote 36 At the federal level, CHI has created a list of companies that offer interoperable systems.Footnote 37
Implement interoperability standards that are not rigid.
Interoperability standards that are too prescriptive can harm competition and undermine innovation. This effect can be most severe when standards:
- Have a high cost of compliance. This is particularly true for small and medium sized companies, who may lack the resources to comply.Footnote 38
- Require the use of technology that is protected by a patent or other intellectual property right. This can cause problems for new companies to obtain the right to use the patent.Footnote 39
- Are based on technologies used by established companies. This can stop entrants from being able to use innovative new ways of serving the marketplace.
- Are rigid. Innovation in data-driven markets can happen quickly. In this case, standards must be flexible to permit such innovation.Footnote 40
- Require every solution to have a specific set of functions. This can limit the ability of entrants to serve customers in different ways.Footnote 41
Interoperability standards should not be burdensome. They ought to be developed with input from both existing companies and companies with plans to enter the industry. This will help to avoid putting rules in place that restrict competition and innovation.
Interoperability standards should allow for flexibility to develop follow-on innovations that are built over-top of existing solutions and systems. Where possible, they should align with international counterparts to promote greater collaboration on research and innovation.
Many groups say Canada should base its interoperability standards on current international standards.Footnote 42 This can enable Canadian companies to build once and compete more effectively in international markets. One example: the HL7 Fast Healthcare Interoperability Resources (FHIR) standard. FHIR is used by several groups in Canada, including CHI and the British Columbia Provincial Health Authority.Footnote 43 In the U.S., it’s used by the Office of the National Coordinator for Health Information Technology.Footnote 44
Use regulatory sandboxes to assess potential risks.
Sharing health data can pose risks to data quality, security and privacy. These risks can be limited by using regulatory sandboxes. They provide a test bed for companies to experiment and test innovations live, under the regulator’s oversight. In doing so, they can reduce barriers to entry and innovation, while minimizing associated risks.Footnote 45
Eventually extend primary health care EMR interoperability standards to others.
Data sharing between primary health care EMR systems is a first step to achieving the seamless sharing of personal health information. However, more complete patient profiles can be made using data held by hospitals, medical labs and other providers. This can produce benefits for quality of patient care, research and innovation. In that regard, data sharing in primary health care EMR systems should be a first step towards broader data sharing with other EMRs, including hospital and specialist EMRs.
Next Steps
Canadians deserve to have access to modern, innovative digital health care solutions. To do that, innovative companies must first be given the ability to offer those kinds of solutions in the Canadian marketplace and a chance to compete for customers. Currently they face barriers preventing them from doing so. One way to reduce those barriers is by making it easier for companies to integrate with primary health care EMRs, with appropriate privacy and security protections in place. This will push digital health care companies to innovate and invest in new products and processes to gain a competitive edge on their rivals and help ensure Canadians have access to modern digital health care solutions.
The Competition Bureau invites Canadian policymakers to review and consider the recommendations made in this report to unlock the power of personal health information in Canada. The COVID pandemic has presented an important crossroad for innovation in health care. We welcome the opportunity to continue working with policymakers to help ensure policies do not unnecessarily impede competition and innovation in this important sector.
How to Contact the Competition Bureau
Anyone wishing to obtain additional information about the Competition Act, the Consumer Packaging and Labelling Act, the Textile Labelling Act, the Precious Metals Marking Act or the Bureau's program of written opinions, or to file a complaint under any of these Acts should contact the Competition Bureau's Information Centre:
Web sitewww.competitionbureau.gc.ca
Address
Information Centre
Competition Bureau
50 Victoria Street
Gatineau, Quebec
K1A 0C9
Telephone
Toll free: 1-800-348-5358
National Capital Region: 819-997-4282
TTY (for hearing impaired): 1‑866‑694‑8389
Facsimile
819-997-0324

